
The AACR Cancer Progress Report 2024 highlights research-driven advances in cancer science and medicine.
Research-driven advances in identifying genetic mutations that fuel tumor growth have set the stage for a new era of precision medicine.
Learn More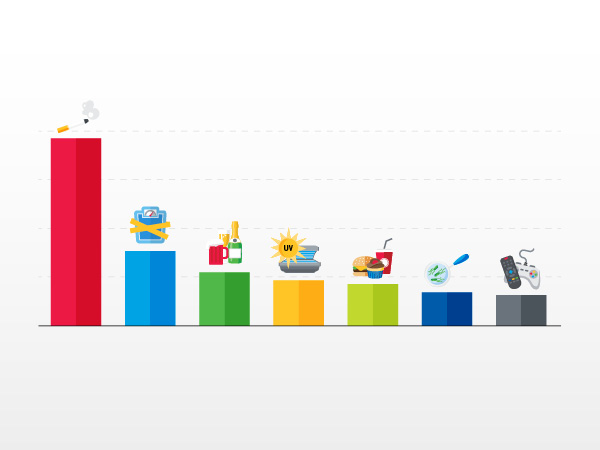
In the United States, 40 percent of all cancers are associated with modifiable risk factors.
Learn More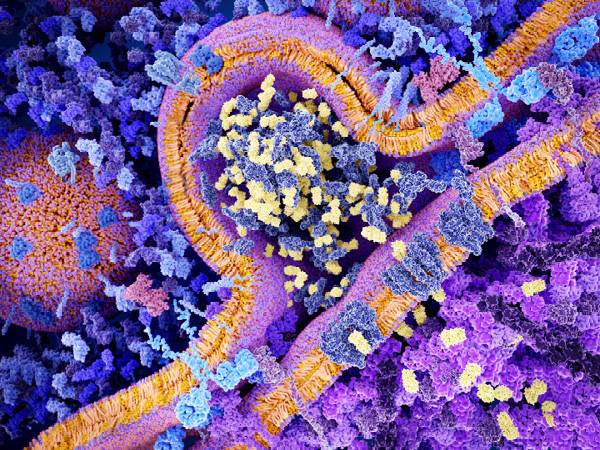
Cancer immunotherapeutics work by unleashing the power of a patient’s immune system to fight cancer and have emerged as one of the most exciting new approaches to cancer treatment.
Learn More

